How Do Tricyclic Antidepressants Work
Tricyclic antidepressants work by directly increasing the levels of norepinephrine and serotonin, but they also block a chemical known as acetylcholine, too. Its the latter effect that probably results in better results for people who dont respond to treatment with SNRIs or SSRIs. Most researchers agree that achieving balance between these three brain chemicals is one of the best ways to reduce pain.
Why These Drugs Are Often Addictive
Steven Gans, MD is board-certified in psychiatry and is an active supervisor, teacher, and mentor at Massachusetts General Hospital.
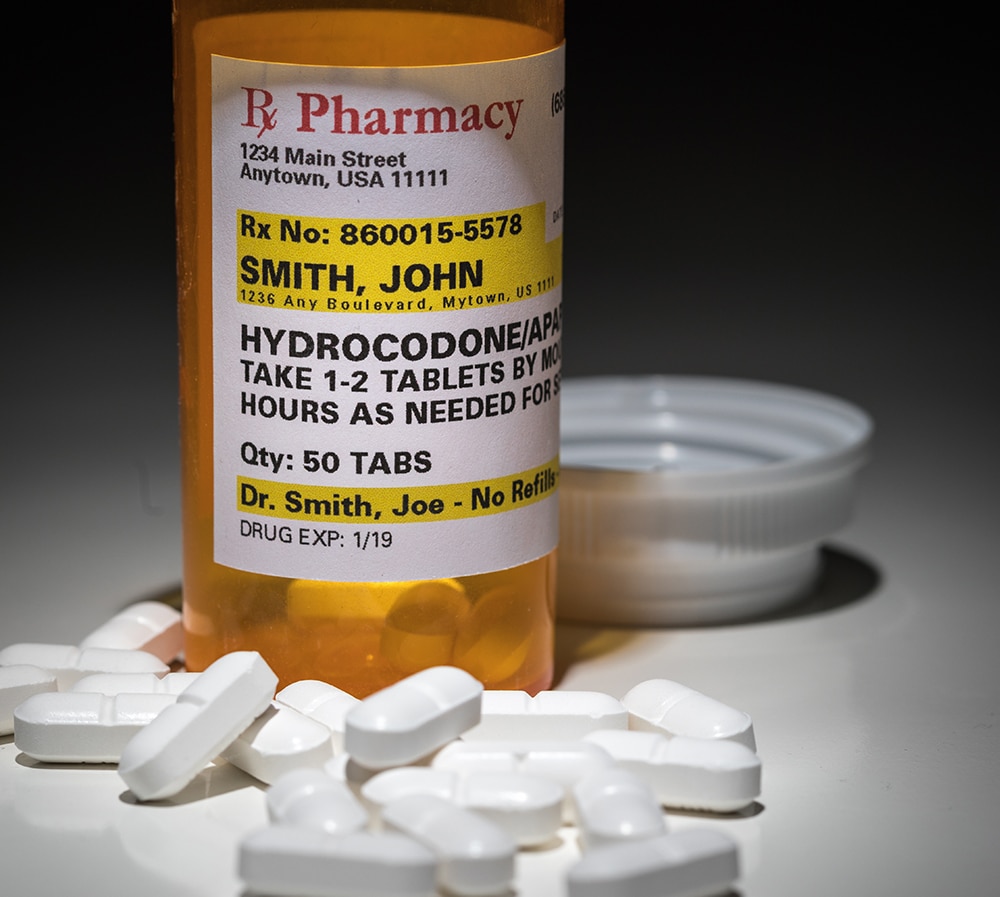
One of the most common reasons Americans visit their doctors is to get help with pain relief. Pain causes distress and can even be debilitating. Doctors sometimes prescribe opioid pain relievers to their patients who are in pain. While these drugs can provide much-needed relief, they also have the potential for misuse and addiction.
Signs And Symptoms Of Opioid Misuse
Unfortunately, the nature of painkillers is that they become less effective over time. This is partly because your body adjusts to the medication and develops a tolerance, which means your body requires higher doses of the drug to get the same effect.
There are certain signs that therapeutic use of opioids has crossed into the territory of addiction.
Verywell / JR Bee
Signs to be aware of include:
- Exhibiting compulsive behaviors to get the drug and continue to use it
- Taking the medication to get high or relieve anxiety rather than to relieve pain
- Needing to take a higher dose of medication to feel the effects previously experienced at lower dosages
- Using pain medication in amounts or at times that are not consistent with a doctor’s prescriptionespecially if someone is misleading their doctor or pharmacist to do so
If you recognize these behaviors in a loved one or are concerned about your own use of pain medication, it’s important to talk to your healthcare provider.
Opioid Addiction Discussion Guide
It has also become common for fentanyl to be used in counterfeit drugs or be cut into illicit drugs such as heroin and cocaine. People using those drugs are often unaware that they contain fentanyl, and just a very small amount can lead to severe illness and even death.
Read Also: Most Individuals With An Opioid Use Disorder Are Addicted To:
Clinical Efforts To Prevent The Acute
There are also many efforts to develop new pain treatments, but there has been less attention devoted to developing interventions that could prevent the acute-to-chronic pain transition, said Robert Dworkin, professor of anesthesiology and perioperative medicine, neurology, and psychiatry at the University of Rochester. Such studies could test various models of prevention, including the following conditions in which the acute-to-chronic pain transition often occurs:
- Surgery, leading to chronic postsurgical pain
- Acute low back injury leading to chronic low back pain
- Wrist fracture, leading to CRPS
- Cancer chemotherapy, leading to peripheral neuropathy
- Herpes zoster and the development of postherpetic neuralgia and
- Diabetic peripheral neuropathy.
The burden of chronic pain associated with these conditions is high, said Dworkin. For example, postsurgical pain persists in between 10 and 50 percent of cases, varying with the type of surgery , although Dworkin said it is unclear whether severe acute pain itself is a causal risk factor or concomitant to nerve or musculoskeletal damage. Mackey added that surgery is nothing more than a controlled injury and thus, the perioperative period provides a unique environment in which to study what happens before and after injury.
More Women Are In Pain

Women are prescribed pain relievers more often than men, says Hammond, who also sees patients at the Center for Addiction and Pregnancy at Johns Hopkins Bayview Medical Center. Part of that has to do with women tending to have lower pain tolerance in general and being more likely to experience chronic pain conditions.
Women suffer from migraine headaches and neck, facial and lower back pain at up to twice the rate men do. In addition, women are more likely to develop conditions that cause chronic pain. For example, women are three times more likely to develop rheumatoid arthritis and four to seven times more likely to develop fibromyalgia than men are.
Another component of women being on higher doses of painkillers and using them for a longer period of time has to do with our culture, explains Hammond. Unfortunately, it has historically been more socially acceptable for women to ask for help, while men may feel they have to just grin and bear it.
Don’t Miss: Can You Get Addicted To Melatonin
Rationale For Evidence Review And What This Review Adds
Requirements in the 2010 Patient Protection and Affordable Care Act led the Department of Health & Human Services to contract with the Institute of Medicine to assess the state of the science on pain research, care, and education and formulate recommendations in these key areas.1,4 Recommendations outlined in the 2011 IOM report have spawned a number of national initiatives to address gaps related to understanding the complexities of pain assessment and management, including the creation of the NPS under the oversight of the Interagency Pain Research Coordinating Committee , and creation of a federal portfolio of existing pain research to help inform additional research needs on pain. Concerns regarding the use of opioids for management of chronic pain are outlined in both the IOM report and the NPS. These initiatives, along with the recent publication of the evidence-based guideline on opioid use for chronic pain by the Centers for Disease Control and Prevention,11 have prompted additional primary research on alternatives to opioids in managing chronic pain.
Signs Of Opioid Dependence And Misuse
Opioid dependence is a term used to describe the way your body adapts and begins needing opioids to avoid negative effects. If you find that youre taking medication more frequently than prescribed say every four hours instead of six or need frequent refills or your pain is not well-managed, you should talk to your doctor, says Hammond. Your body could be developing a tolerance to the drug, which makes you need more medication to achieve the same pain relief.
Another sign of opioid dependence is experiencing withdrawal symptoms in the absence of medication, such as:
- Agitation and anxiety
- Abdominal cramping and diarrhea
- Nausea and vomiting
Misuse typically refers to behavior associated with drug use. If you find youre using prescription opioids for the feeling it gives you instead of pain control, thats a sign of an opioid use disorder, or addiction. If you cant stop using the drugs despite negative consequences at work, school and home, thats also a clear sign of a problem.
Recommended Reading: How To Get Rid Of Fast Food Addiction
When Are Snris And Ssris Indicated
As some chronic pain patients experience depression and/or anxiety after extended bouts with pain, some doctors are proactive about treating pain with SNRIs and SSRIs. Others prefer to use it only when the ability to treat pain exceeds over-the-counter options. Both are most commonly used to treat these conditions:
- Spinal cord injuries
- Certain traumatic brain injuries
SNRIs and SSRIs arent addictive, but they may not be right for everyone. They are contraindicated in patients with a history of suicidal thoughts and those with bipolar disorder. They also cannot be taken with MAO inhibitors, other serotonin-boosting drugs, or pain drugs like Tramadol that may also have a weak effect on serotonin levels. Your doctor can help you to calculate the best dose for your condition.
Withdraw From Pain Medications
When you have been in chronic pain, it can severely impact all aspects of your life. Trauma and injuries often necessitate pain medication. Any surgeries you may have had might have led you to need pain medication as well. Over time, pain medications, particularly opioid based medications, can lead to dependence.
When you become dependent on pain medication, if you stop taking the medication you will experience symptoms of withdrawal. This can happen to anyone who has relied on pain medication in order to relieve debilitating symptoms. Unfortunately, in addition to withdrawal symptoms, you may also experience a rebound of intense pain while you are detoxing from the pain medication. This can make it almost impossible to stop using on your own.
If you have found yourself experiencing withdrawal symptoms and rebound pain, you will need professional help from addiction specialists in order to recover from your dependence. The first step in your recovery will involve detoxing from the medication. Our addiction professionals will be able to provide supportive care during detox so that your concerns are heard and your needs are met.
Also Check: How To Combat Drug Addiction
Biomarkers: A Bridge To Clinical Studies
In drug discovery for any condition, typically many targets are identified and supported by genetic associations and studies in animal models, said Andrew Ahn. He said the next step requires an important translational leap to enter the framework of clinical opportunity within the pharmaceutical industry. Biomarkers can offer an opportunity to reach across that divide, he said, noting that partnerships are essential in this area given that pharmaceutical companies may not have all the expertise needed to identify mechanisms, connect them to a disorder, and develop tools and assays to move from a mechanistic hypothesis to druggable targets and eventually, novel compounds.
Many workshop participants noted that objective markers are needed to demonstrate clinical efficacy of pain medications in development. Currently, the most commonly used pain assessment measures are subjective visual analog and numerical pain rating scales, said Tor Wager.
Scientists Search For A Safe Non
With the support of the National Institute on Drug Abuse, scientists at Wake Forest School of Medicine have been working to find a safe, non-addictive pain killer to help fight the current opioid crisis in this country. And they may have done just that, though in an animal model. Known as AT-121, the new chemical compound has dual therapeutic action that suppressed the addictive effects of opioids and produced morphine-like analgesic effects in non-human primates.
In our study, we found AT-121 to be safe and non-addictive, as well as an effective pain medication, said Mei-Chuan Ko, Ph.D., professor of physiology and pharmacology at the School of Medicine, part of Wake Forest Baptist Medical Center. In addition, this compound also was effective at blocking abuse potential of prescription opioids, much like buprenorphine does for heroin, so we hope it could be used to treat pain and opioid abuse.
The work was supported by grants from the National Institutes of Health, National Institute on Drug Abuse R01DA032568, R01DA027811, R44DA042465, R21DA040104, and R21DA044775, and the U.S. Department of Defense W81XWH-13-2-0045.
Read this article on ScienceDaily: Wake Forest Baptist Medical Center. Scientists take big step toward finding non-addictive painkiller. ScienceDaily. ScienceDaily, 29 August 2018. www.sciencedaily.com/releases/2018/08/180829143821.htm.
You Might Also Enjoy…
Don’t Miss: How To Treat Marijuana Addiction
A Targeted Approach To Therapy Development In The Clinical Space
A targeted approach to therapy development when drugs are developed and tested in strongly phenotyped, well-defined populations could represent a potentially useful foundational strategy on which to build a publicprivate partnership, suggested Koroshetz. Sharon Hertz, director of the Division of Anesthesia, Analgesia, and Addiction Products at the Food and Drug Administration’s Center for Drug Evaluation and Research, agreed that defining a subpopulation that is more likely to respond to a drug, and then demonstrating efficacy in that subpopulation, may be a good drug development strategy. However, if a compound in development does not target a specific aspect of a specific disease, and the drug is anticipated ultimately to be used in a more general way, there are dangers to that approach, said Hertz.
Usc Michelson Center Scientists Are Part Of An International Team Developing New Alternatives To Easing Pain In The Midst Of A National Crisis
What if scientists could develop an opioid-based painkiller that is not addictive and has limited side effects?
That is possible based on new findings by an international team of scientists that included contributions from top researchers at the Bridge Institute at the USC Michelson Center for Convergent Bioscience.
The international team captured the crystal structure of the kappa opioid receptor critical for providing pain relief in action on the surface of human brain cells. The researchers also made another important discovery: a new opioid-based compound that, unlike current opioids, activates only the kappa opioid receptor, raising hopes that they may develop a painkiller that has no risk of addiction and, therefore, none of the devastating consequences and side effects that accompany it.
The findings were published Jan. 4 in the journal Cell. They are an example of how USC Michelson Center scientists collaborate with a range of experts in multiple disciplines to conduct groundbreaking research, including the opioid addiction.
Read Also: How To Stop Pleasure Addiction
Are There Pain Medications That Arent Habit Forming
America is in the midst of an epidemic of pain medication abuse. The problem is the addictive nature of prescription opioids: a recent report from the Trust for Americas Health found double- and triple-digit increases in synthetic opioid deaths from 20162017 of both males and females, from all ethnicities, and in every region of the nation. The lesser known treatments are these non habit forming pain medications.
Pain is frustrating and debilitating, and it can take over your life without warning. Unfortunately, opioid-based pain medications can be addictive, which can cause an entirely new set of problems.
It isnt always simple to manage pain without habit-forming medications, or it wouldnt be the problem it is but there are alternatives. The knowledge to protect yourself and your loved ones is more important today than ever before.
New Hope For Treating Chronic Pain Without Opioids
- Share on:
According to some estimates, chronic pain affects up to 40% of Americans, and treating it frustrates both clinicians and patientsa frustration thats often compounded by a hesitation to prescribe opioids for pain.
A new study from the University of Michigan School of Dentistry confirms that a low dose of a drug called naltrexone is a good option for patients with orofacial and chronic pain, without the risk of addiction, said first author Elizabeth Hatfield, a clinical lecturer in the Department of Oral and Maxillofacial Surgery and Hospital Dentistry.
Naltrexone is a semisynthetic opioid first developed in 1963 as an oral alternative to naloxone, the nasal spray used to reverse opioid drug overdoses. When prescribed at doses of 50 to 100 milligrams, naltrexone blocks the effects of alcohol and opioids.
Low-dose naltrexone has been used off-label for years to treat chronic pain, but Hatfield said this is the first in-depth, systematic review of the literature to determine if the drug is indeed a good option for patients and deserving of more formal study.
We found a reduction in pain intensity and improvement in quality of life, and a reduction in opioid use for patients with chronic pain, said Hatfield, who hopes to initiate a randomized control trial of low dose naltrexone.
The study appears in the Journal of the American Dental Association.
More information:
Don’t Miss: How To Help Addicts In Recovery
A Solution To Painkiller Addiction
Opioids, such as morphine et loxycodonecan cause a addiction. As only one type of G protein is activated by BnOCPA, its actions are very selective which minimizes the possibility of develop addictive behaviors.
The researchers were pleasantly surprised to note the selectivity of the molecule. It would make it possible to develop a new type of painkiller much more beneficial to health. Additionally, it would help more easily target receptors which are essential for the treatment of various diseases.
Nonaddictive Drug Compound Could Replace Opioids For Chronic Pain Sufferers
WEST LAFAYETTE, Ind. A new nonaddictive drug compound discovered by Purdue University researchers could lead to the treatment of chronic pain without the need to rely on opioids, just as a bipartisan package of bills moves through the U.S. House and Senate to battle the nations opioid epidemic.
A compound developed by a research team led by Val Watts, professor of medicinal chemistry and molecular pharmacology and associate dean for research in Purdues College of Pharmacy, shows unparalleled selectivity in inhibiting the adenylyl cyclase 1 , making it a potential target for treating pain and reducing the dependency on opioids for pain management.
This compound shows promise in inhibiting one class of AC1, which could decrease physical symptoms of opioid addiction withdrawal, and that could help reduce psychological dependence, Watts said.
Last year, the U.S. Department of Health and Human Services regarding the spike in opioid overdoses. In 2016, 116 people died each day from opioid-related drug overdoses. According to the Centers for Disease Control and Prevention, overdose deaths involving prescription opioids have quadrupled since 1999. From 1999 to 2015, more than 183,000 people have died in the United States from overdoses related to prescription opioids. Watch a video from the CDC about opioids here.
Also Check: How To Stop Food Addiction And Emotional Eating
Key Question 1 Effectiveness And Comparative Effectiveness
The Science Behind 194
Dr. Khannas prior research identified a protein, collapsin response mediator protein 2 , and an enzyme, Ubc9, that both play a role in NaV1.7 activation. CRMP2 is a protein that binds to NaV1.7 and transports it to the cell membrane, where sodium ions are then transferred into the cell. Ubc9 is an enzyme that tags CRMP2 with another protein a small ubiquitin-like modifier protein to specifically direct control of NaV1.7.
Building on this knowledge, Dr. Khanna and the team set out to determine if they could directly regulate the activity of NaV1.7 by blocking Ubc9 from interacting with CRMP2. Team members including May Khanna, PhD, associate professor of pharmacology and BIO5 Institute member, Vijay Gokhale, PhD, associate research professor in the BIO5 Institute, and Samantha Perez-Miller, PhD, researcher and scientist in the Department of Pharmacology, examined 50,000 existing small molecules to identify the ones with a structure similar to Ubc9.
They selected less than 50 of the closest matches, which were then tested in Dr. Khannas laboratory to see if their presence would suppress the influx of sodium through NaV1.7. The findings were promising, so the team set their sights on developing a unique, more effective compound.
It is an important step in optimizing the compounds potential as a pain-relieving drug and advancing to the next stage, where researchers will file for Food and Drug Administration approval to begin clinical trials.
Related Stories
Read Also: Why Do Some People Have Addictive Personalities
